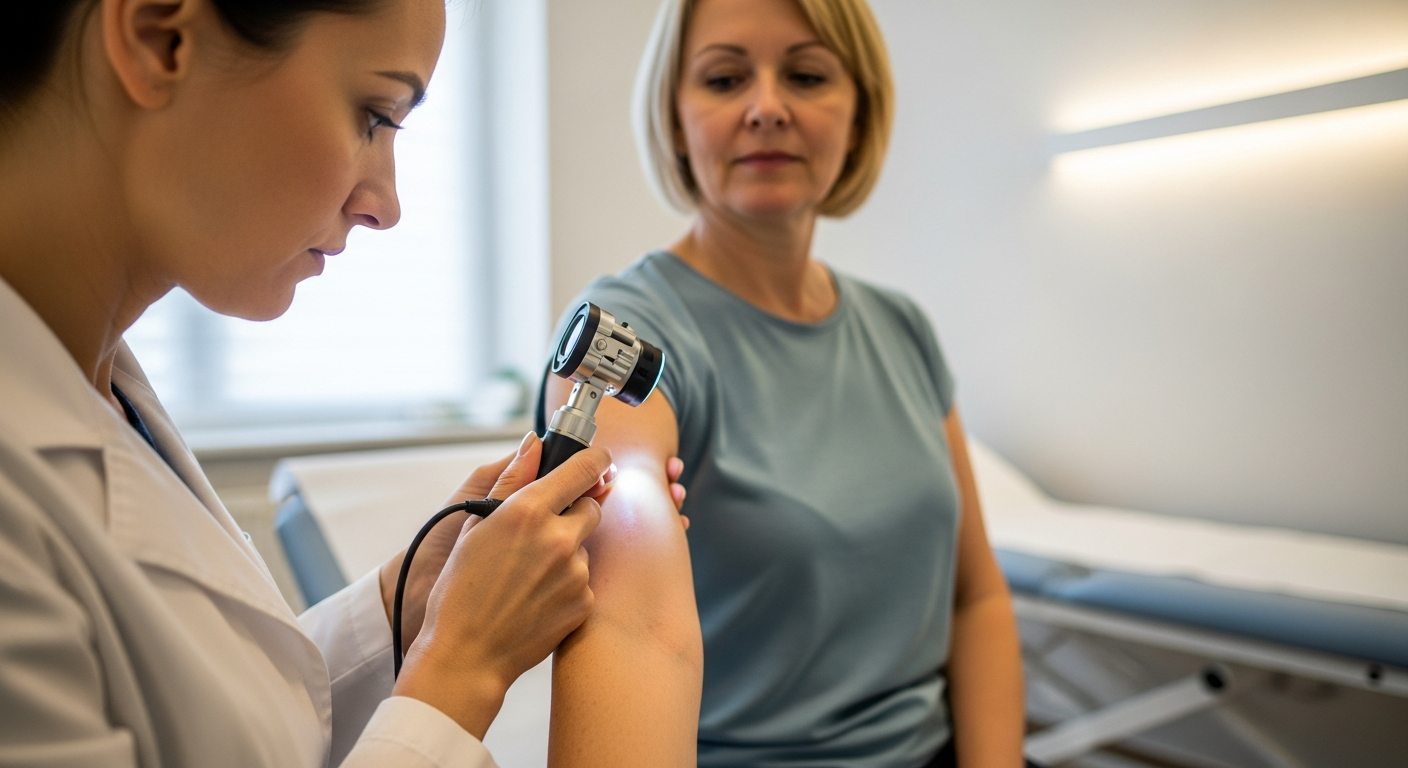
Unnoticed Triggers That Could Result in Tardive Dyskinesia
Tardive dyskinesia is a movement disorder that can develop gradually, often after long-term use of certain medications. Because early changes in facial or body movements may appear subtle, they are sometimes overlooked or mistaken for temporary side effects. Understanding potential triggers and risk factors helps clarify when unusual movements warrant medical review and discussion.
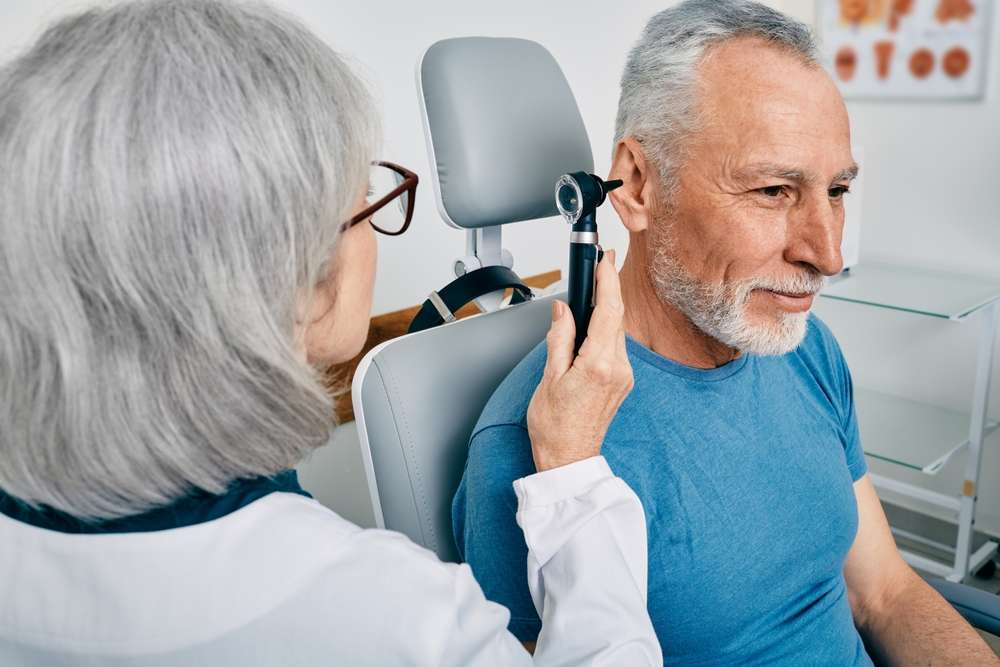
Tardive dyskinesia is a movement disorder that can appear after months or years of exposure to dopamine blocking medicines. Many triggers are easy to overlook, from cumulative medication dose to coexisting health conditions. Recognizing patterns early can support timely evaluation and tailored treatment in your area.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Which medications are commonly implicated, and how does long-term use raise risk
- First generation antipsychotics: haloperidol, chlorpromazine, fluphenazine. Higher potency and higher total exposure tend to increase risk.
- Second generation antipsychotics: risperidone, olanzapine, quetiapine, aripiprazole, ziprasidone. Although often used for fewer movement effects than older agents, tardive dyskinesia can still occur, especially with sustained use.
- Antiemetics that block dopamine: metoclopramide and prochlorperazine. Metoclopramide carries a boxed warning in the United States advising against use beyond 12 weeks in most cases due to risk of tardive dyskinesia.
- Cumulative exposure matters: longer duration, higher daily doses, and use of multiple dopamine blocking agents increase overall risk.
- Route and formulation: long acting injectable antipsychotics can contribute to ongoing exposure even after a dose change, which may delay symptom improvement.
Early movement changes that may signal developing tardive dyskinesia
- Repetitive facial movements such as lip smacking, puckering, or chewing motions without food.
- Tongue movements including darting, rolling, or frequent pressing against teeth or cheeks.
- Rapid blinking, grimacing, or eyebrow lifting that feels hard to control.
- Subtle hand or finger motions such as piano playing movements or persistent fidgeting.
- Foot tapping, ankle rotations, or knee bouncing while seated at rest.
- Rocking of the trunk or hips, or swaying when standing still.
- Sounds like soft grunts or throat clearing unrelated to illness.
- Clues from daily life, such as trouble keeping dentures in place or new difficulties with speaking or eating.
These movements often emerge gradually, are more noticeable at rest, and may lessen during purposeful activity, making them easy to miss early on.
Factors that can influence an individual’s susceptibility
Several elements can raise vulnerability to tardive dyskinesia. Age is a key factor, with older adults generally at higher risk. A history of movement side effects on antipsychotics, such as acute dystonia or parkinsonism, signals increased susceptibility. Women, particularly after menopause, appear to be at higher risk. Metabolic conditions like diabetes can heighten vulnerability, as can nutritional deficiencies and significant weight loss.
Medication related variables also matter. Higher cumulative dose, rapid dose escalations, and use of high potency antipsychotics increase the likelihood of symptoms. Co prescribing anticholinergic drugs for stiffness or tremor may mask early warning signs, delaying recognition. Genetics and differences in drug metabolism can influence exposure at typical doses, meaning two people on the same regimen may face different risks.
Why symptoms may persist even after medication adjustments
Tardive dyskinesia is thought to involve dopamine receptor supersensitivity and changes within motor circuits of the brain that develop over time. Because those adaptations do not reverse quickly, reducing the dose or switching medications may not lead to immediate improvement. Some individuals experience lingering symptoms for months, and in others changes can be long lasting.
Ongoing exposure from long acting injections or residual drug levels can also sustain movements after a prescription change. Stress, sleep disruption, caffeine, and nicotine may transiently intensify movements, making progress harder to judge. Evidence based treatments such as VMAT2 inhibitors including valbenazine and deutetrabenazine are used in the United States to reduce involuntary movements, while clozapine is sometimes considered in patients who still require an antipsychotic and have not improved with other strategies. Physical, speech, and occupational therapy can help with daily function and safety.
When involuntary movements should prompt a clinical evaluation
Seek a clinical assessment if any new, repetitive, or hard to control movements appear while taking an antipsychotic or a dopamine blocking antiemetic, even if mild. A clinician can perform structured exams such as the Abnormal Involuntary Movement Scale to track changes over time. Evaluation is especially important if movements interfere with eating, speaking, work, or sleep; if falls, biting of the tongue or inner cheeks, or social withdrawal occur; or if symptoms persist beyond a few weeks despite medication changes.
When arranging care in the United States, consider contacting your prescribing clinician, primary care, or a neurologist or psychiatrist familiar with movement disorders. Local services in your area, including hospital clinics and community mental health centers, can coordinate medication review, ongoing monitoring, and supportive therapies. Keeping a brief movement diary or short video clips can help clinicians appreciate patterns across the day.
Understanding the interplay of medication exposure, individual susceptibility, and early signs can make a meaningful difference. While not every case can be prevented, regular monitoring, prudent prescribing, and timely evaluation offer the best chance to minimize impact and support daily life.