Unexpected Causes of Tardive Dyskinesia You Should Know
Tardive Dyskinesia (TD) is often linked to long-term use of certain medications, but the full picture is more complex. Subtle risk factors, individual vulnerability, dosage patterns, and underlying health conditions may quietly increase the likelihood of developing involuntary movements. Understanding these less visible triggers can help patients and caregivers recognize risks earlier and seek timely medical guidance.
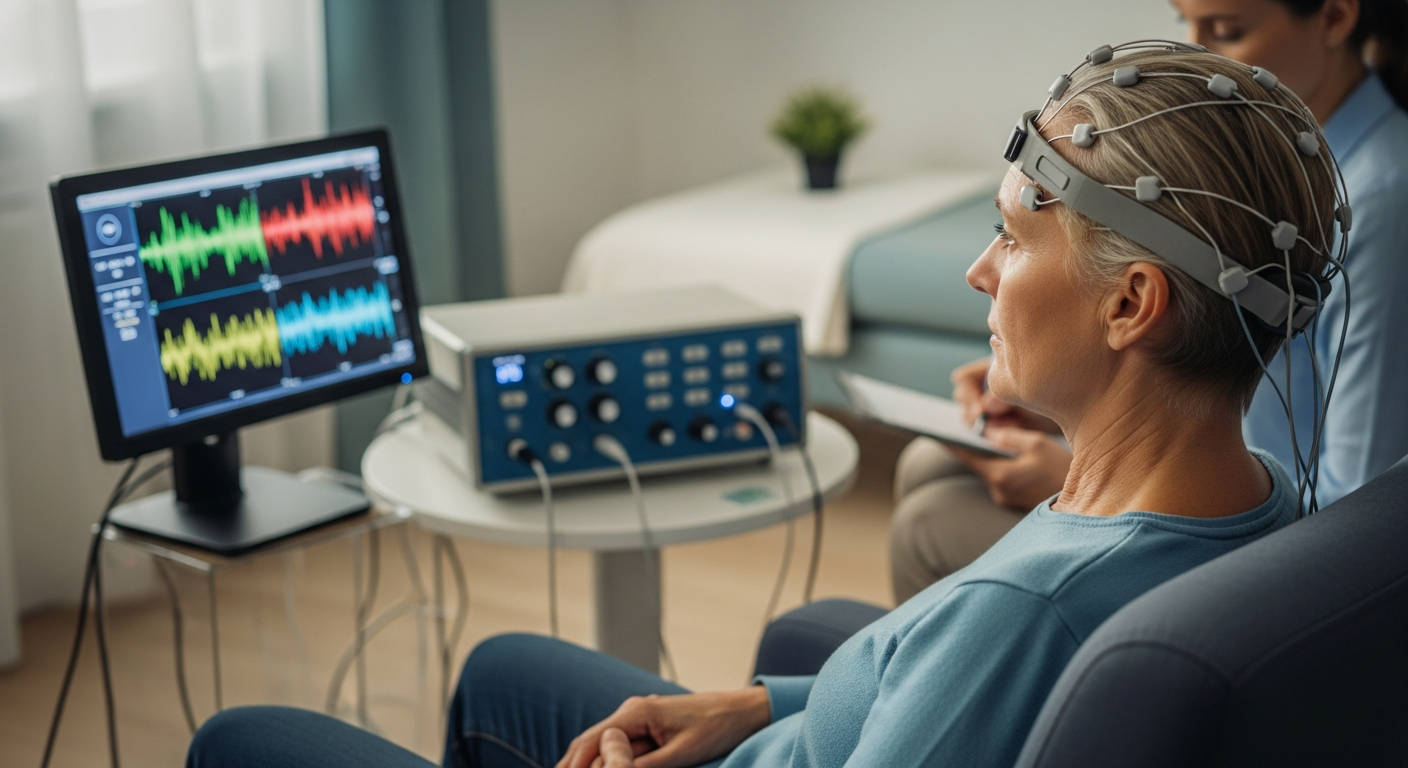
Tardive dyskinesia manifests through uncontrollable movements of the face, tongue, lips, and sometimes limbs. These involuntary motions can range from mild to severe, affecting speech, eating, and daily activities. The condition typically develops after prolonged exposure to dopamine-blocking medications, but emerging research reveals additional contributing factors that deserve attention. Recognising these diverse causes empowers patients and healthcare providers to take proactive measures in reducing risk and identifying symptoms early.
Medication-Related Risk Factors
Antipsychotic medications remain the primary culprits in tardive dyskinesia development, particularly older first-generation drugs like haloperidol and chlorpromazine. However, newer second-generation antipsychotics, though associated with lower risk, can still trigger the condition. Beyond antipsychotics, certain medications prescribed for gastrointestinal disorders, such as metoclopramide used for nausea and reflux, carry significant risk when used long-term. Anti-nausea drugs like prochlorperazine also block dopamine receptors and may contribute to movement disorders. The duration and dosage of these medications directly correlate with increased susceptibility. Patients taking these drugs for extended periods, particularly beyond three months, face elevated risk. Abrupt discontinuation or dosage changes can sometimes unmask underlying movement disorders that were suppressed during active treatment. Healthcare providers must carefully weigh the benefits against potential neurological complications when prescribing dopamine-blocking medications, especially for chronic conditions. Regular monitoring and periodic reassessment of medication necessity help minimise exposure and reduce the likelihood of developing this debilitating condition.
Individual and Biological Vulnerabilities
Certain individuals possess inherent characteristics that increase their susceptibility to tardive dyskinesia, regardless of medication exposure. Age plays a crucial role, with older adults showing significantly higher risk due to natural changes in brain chemistry and reduced dopamine receptor density. Women, particularly postmenopausal women, demonstrate greater vulnerability compared to men, possibly due to hormonal influences on dopamine systems. Genetic factors also contribute, as some people possess variations in genes responsible for drug metabolism and neurotransmitter regulation. Those with pre-existing neurological conditions, including Parkinson disease or other movement disorders, face compounded risk when prescribed dopamine-blocking medications. Diabetes and other metabolic conditions have been linked to increased susceptibility, though the exact mechanisms remain under investigation. Individuals with a history of substance abuse, particularly alcohol dependence, may experience altered brain chemistry that heightens vulnerability. Cognitive impairment and dementia also correlate with higher incidence rates. Brain injury or stroke survivors show elevated risk, as damage to motor control regions may predispose them to movement disorders. Understanding these biological vulnerabilities allows for more personalised risk assessment and closer monitoring of at-risk populations during medication therapy.
Early Warning Signs and Prevention Strategies
Recognising the earliest manifestations of tardive dyskinesia enables timely intervention and potentially reversible outcomes. Initial symptoms often include subtle facial movements such as lip smacking, tongue protrusion, or rapid eye blinking that may be dismissed as nervous habits. Patients might notice difficulty controlling facial expressions or experience involuntary chewing motions. Finger movements, hand clenching, or foot tapping can signal early onset. Family members often detect these changes before patients themselves become aware. Prevention begins with judicious prescribing practices, using the lowest effective medication dose for the shortest necessary duration. Regular neurological assessments, ideally every three to six months for patients on long-term dopamine-blocking drugs, help identify emerging symptoms. The Abnormal Involuntary Movement Scale provides a standardised tool for monitoring. When possible, healthcare providers should consider alternative treatments with lower neurological risk profiles. Patients prescribed high-risk medications should receive thorough education about warning signs and the importance of reporting new involuntary movements immediately. Early detection sometimes allows for medication adjustment or discontinuation before symptoms become permanent. Lifestyle factors, including stress management and adequate sleep, may support overall neurological health. While no guaranteed prevention method exists, awareness and vigilance significantly improve outcomes. Collaborative decision-making between patients and healthcare providers ensures that treatment benefits justify potential risks, with ongoing evaluation throughout the medication course.
Treatment Approaches and Management Options
When tardive dyskinesia develops, several management strategies can help reduce symptoms and improve quality of life. The first step typically involves reviewing and potentially discontinuing or switching the causative medication, though this decision requires careful medical supervision as abrupt changes can worsen symptoms temporarily. Two medications specifically approved for tardive dyskinesia treatment include valbenazine and deutetrabenazine, which work by reducing dopamine signalling. These treatments have demonstrated effectiveness in clinical trials, though individual responses vary. Some patients benefit from vitamin E supplementation, particularly when started early, though evidence remains mixed. Ginkgo biloba has shown promise in some studies but requires further research. Botulinum toxin injections may provide relief for localised symptoms affecting specific muscle groups. Physical therapy and speech therapy help patients adapt to movement challenges and maintain functional abilities. Psychological support addresses the emotional impact of living with involuntary movements, which can cause social anxiety and reduced self-esteem. Dietary considerations, including antioxidant-rich foods, may support neurological health. Regular exercise promotes overall wellbeing and may help with motor control. Support groups connect individuals facing similar challenges, providing practical coping strategies and emotional validation. Management requires a comprehensive, individualised approach addressing both physical symptoms and psychosocial impacts.
Long-Term Outlook and Quality of Life Considerations
The progression and severity of tardive dyskinesia vary considerably among individuals. Some experience mild symptoms that stabilise or even improve over time, particularly when causative medications are discontinued early. Others face persistent or progressive symptoms that significantly impact daily functioning. Younger patients generally show better recovery potential compared to older adults. The condition can affect employment, social relationships, and self-image, making comprehensive support essential. Workplace accommodations may help individuals maintain employment despite movement challenges. Social stigma surrounding involuntary movements often creates additional psychological burden, highlighting the need for public awareness and understanding. Family education ensures that loved ones provide appropriate support without inadvertently reinforcing self-consciousness. Adaptive strategies, such as timing social activities during periods of reduced symptom severity, help maintain social connections. Technology aids, including communication devices for those with speech difficulties, enhance independence. Regular follow-up with healthcare providers ensures ongoing symptom monitoring and treatment optimisation. Research continues into new therapeutic approaches, offering hope for improved management options. While tardive dyskinesia presents significant challenges, many individuals successfully adapt and maintain meaningful, fulfilling lives through comprehensive care, support systems, and personal resilience.
Understanding the unexpected causes and risk factors associated with tardive dyskinesia empowers individuals and healthcare providers to make informed decisions about medication use and monitoring. Early recognition of warning signs, combined with appropriate prevention strategies, offers the best opportunity for minimising impact and preserving quality of life for those at risk.




