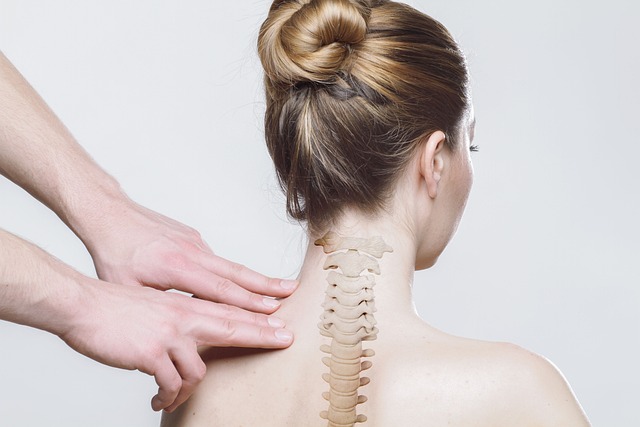
Understanding Early HIV Symptoms and Appropriate Testing Timing
Early HIV symptoms can be subtle and temporary, which makes them easy to mistake for common viral illnesses. Signs such as fever, fatigue, sore throat, or swollen lymph nodes may develop a few weeks after exposure and then gradually resolve. Being aware of these early changes can help determine when testing is appropriate, supporting informed decisions about personal health and reducing the risk of unknowingly transmitting the virus.HIV infection develops in stages, and early symptoms often emerge within weeks of initial exposure. These first signs vary from person to person, and some individuals may not notice any symptoms during the acute phase. Recognizing potential indicators and understanding when testing is recommended can encourage timely action and proactive health management.
Noticing unusual fatigue, fever, or a sore throat after a potential exposure can be stressful, especially because early HIV can resemble common viral infections. Understanding how symptoms typically show up, what they can and cannot tell you, and when different tests become accurate helps you make decisions based on evidence rather than guesswork.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Early Warning Signs in the Body Related to HIV
Early HIV symptoms, when they occur, are often linked to the body’s initial immune response as HIV begins to replicate. People may notice fever, swollen lymph nodes, sore throat, muscle aches, headaches, night sweats, or a new rash. Some also report mouth sores or gastrointestinal symptoms like nausea or diarrhea. These signs are sometimes grouped under “acute HIV infection.” Importantly, many people have mild symptoms or none at all, so the absence of noticeable changes does not rule out infection.
Common Early Signs That Mimic Other Conditions
A key challenge is that common early signs that mimic other conditions are not specific to HIV. The same symptom pattern can appear with influenza, COVID-19, mononucleosis (mono), strep throat, or other viral syndromes. Even a rash can be triggered by medications, allergies, or other infections. Because symptom overlap is so broad, self-diagnosis based on early warning signs can lead to false reassurance or unnecessary panic. Testing is the only reliable way to confirm HIV status after a possible exposure.
Timeline of Early Signs After Possible Exposure
The timeline of early signs after possible exposure varies. When symptoms occur, they often appear about 2–4 weeks after exposure, but a wider range is possible. Symptoms may last several days to a couple of weeks and then resolve, even without treatment—this can happen as the immune system partially controls the initial surge of virus. However, symptom timing does not reliably match testing accuracy timing. Some tests can detect HIV before symptoms start, while others may not detect it until after symptoms have ended.
Why Testing Matters Even After Symptoms Subside
Why testing matters even after symptoms subside comes down to two realities: symptoms can disappear while HIV remains, and early knowledge changes health decisions. Without testing, a person may assume a passing illness means “everything is fine,” when in fact HIV could still be present and gradually affecting immune function. Testing also helps guide safer choices while results are pending, such as using condoms and not sharing injection equipment. If you test too early for the type of test used, a follow-up test may be recommended to confirm the result.
How Early Awareness and Testing Protect Long-Term Health
How early awareness and testing protect long-term health is closely tied to medical monitoring and timely care. HIV is manageable with modern treatment, and earlier diagnosis supports earlier evaluation, baseline lab work, and discussion of treatment options. Early diagnosis also reduces the chance of unknowingly passing HIV to others, because people who know their status can take effective risk-reduction steps and, if diagnosed, can work with clinicians on strategies that support viral suppression.
A practical testing approach is to match the test type to the time since exposure. In the United States, many clinics offer laboratory-based antigen/antibody tests (often called “4th-generation” tests), which can typically detect infection earlier than antibody-only tests. Nucleic acid tests (NATs) can detect HIV even earlier in some cases, but they are not used for every situation and may be ordered based on risk and clinical judgment. At-home tests are accessible and useful, but some are antibody-only and may require more time after exposure to become reliable. If you are unsure which test you received, ask the clinic or check the package insert for the testing window.
If you think you were exposed very recently, it may also be appropriate to ask a clinician about post-exposure prophylaxis (PEP), which is time-sensitive and generally needs to be started as soon as possible after exposure. Separately, people with ongoing risk may consider pre-exposure prophylaxis (PrEP) for future protection. These decisions are individualized and depend on the type of exposure, timing, and personal health factors, so professional guidance is important.
In day-to-day terms, the most helpful mindset is to treat symptoms as a reason to test, not a way to diagnose. Keep track of dates: the date of the possible exposure, the date symptoms began (if any), and the date of each test. If an initial test is negative but taken during an early window period, follow-up testing can be the step that provides a clear answer. Clinics can also recommend testing for other sexually transmitted infections, since symptoms and risks can overlap.
Finally, remember that anxiety after a scare is common, and information can reduce uncertainty. Choosing an appropriate test at the appropriate time, and repeating it when advised, is what turns a confusing set of symptoms into a clear, actionable result. That clarity supports both personal health and the health of partners, regardless of what the final result shows.