Financial Planning for Sleep Therapy Equipment in 2026
Managing the financial aspects of sleep therapy requires careful consideration of diagnostic procedures and equipment maintenance. In New Zealand, patients often navigate a mix of public funding and private expenses. Understanding the projected costs for 2026 helps individuals plan their healthcare budget effectively while ensuring they receive the necessary therapy for long-term well-being and health stability.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Sleep health is a significant concern that affects thousands of New Zealanders, impacting daily energy levels and long-term cardiovascular health. As we look toward 2026, the landscape of therapy equipment and diagnostic services continues to evolve. Financial planning for these essential medical needs involves understanding the various pathways for diagnosis, the ongoing costs of machinery, and the available support systems within the local healthcare framework. Preparing for these costs early can help mitigate the stress of managing a chronic condition while ensuring high-quality care is maintained over time.
Sleep apnea test NZ cost 2026
The journey to effective therapy begins with an accurate diagnosis, which typically involves a sleep study or diagnostic test. In New Zealand, patients can access these tests through the public health system or via private clinics. While public pathways are available at no direct cost to the patient, wait times can be significant, leading many to seek private alternatives. For 2026, the estimated cost for a private home-based sleep test is expected to range between $200 and $600, depending on the complexity of the monitoring required. These tests monitor breathing patterns, oxygen levels, and heart rate during sleep to determine the severity of the condition. Choosing a private test often provides faster results, allowing for quicker initiation of therapy, which can be crucial for those in safety-sensitive occupations or those experiencing severe daytime fatigue.
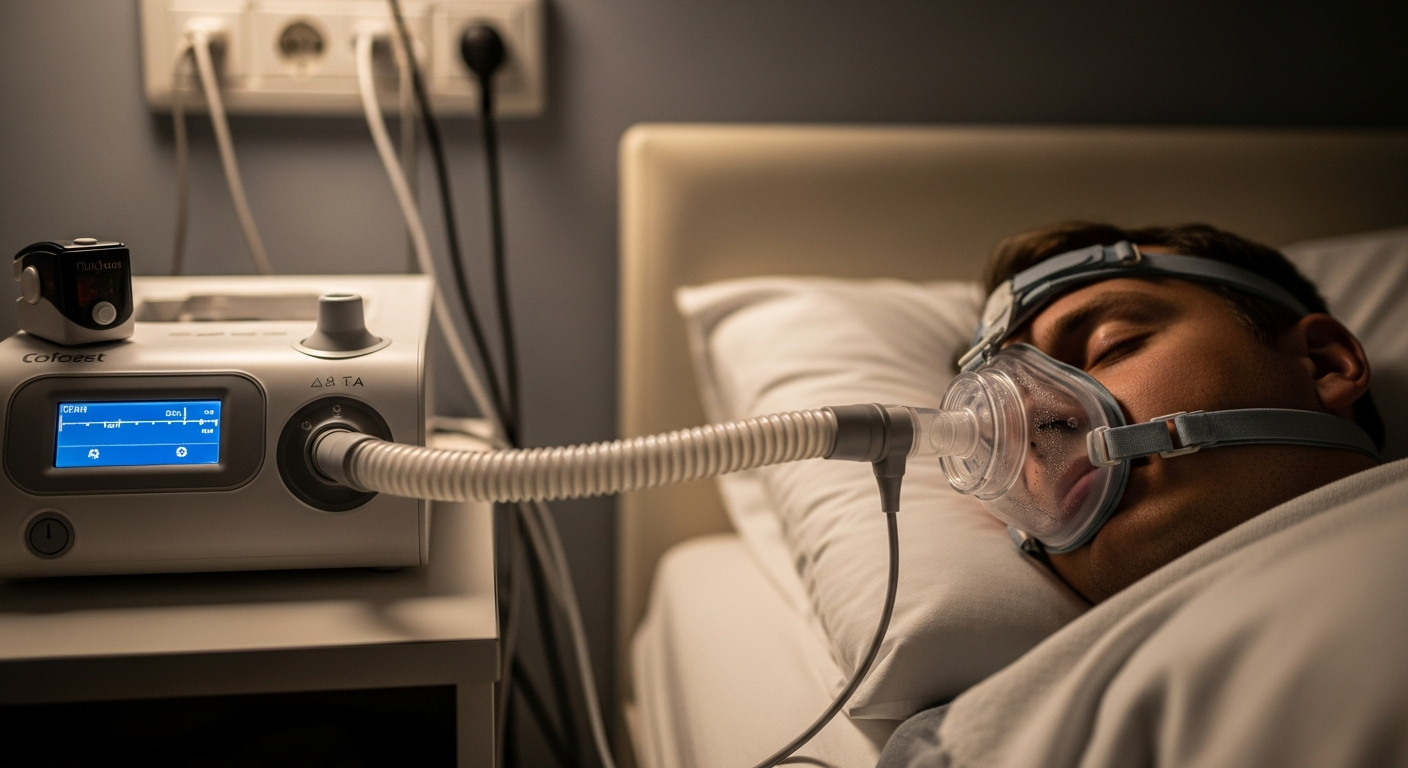
CPAP machine prices NZ reviews
Once a diagnosis is confirmed, the primary treatment often involves Continuous Positive Airway Pressure (CPAP) therapy. The cost of these machines varies based on technology, such as whether the device is a fixed-pressure model or an automatic adjusting (Auto-CPAP) model. In the New Zealand market, reviews often highlight the durability and quiet operation of modern devices. For 2026, individuals should budget between $1,200 and $2,800 for a new machine. This price typically includes the base unit and a humidifier, but masks and tubing are often sold separately. Reviews of equipment from manufacturers like Fisher & Paykel and ResMed suggest that while the initial investment is high, the longevity of these devices—often lasting five to seven years—provides good value. It is also important to factor in the cost of consumables like filters and water chambers, which require regular replacement to ensure the machine functions efficiently and hygienically.
Government funding for CPAP NZ 2026
Navigating government funding is a vital step for many New Zealanders looking to manage the costs of sleep therapy. Te Whatu Ora (Health New Zealand) provides funding for equipment to patients who meet specific clinical criteria, usually based on the severity of their condition and the potential for health improvement. This funding is typically administered through local hospital respiratory departments. Additionally, for those who do not meet the strict hospital criteria but are on low incomes, Work and Income (WINZ) may provide assistance through the Disability Allowance or specialized grants. In 2026, the focus of public funding remains on high-risk individuals, meaning those with mild symptoms may still need to explore private purchase options or payment plans offered by local providers. Understanding the specific requirements of your local health district is essential, as funding availability and waitlists can vary between regions.
Beyond the initial purchase of a machine, long-term financial planning should account for the replacement of masks and accessories. Masks generally need to be replaced every 6 to 12 months due to the degradation of silicone seals, which can lead to leaks and reduced therapy effectiveness. In New Zealand, a high-quality mask can cost between $200 and $450. Furthermore, annual clinical reviews with a sleep physiologist or specialist are recommended to ensure the pressure settings remain optimal for the patient’s changing needs. These consultations, if done privately, add an ongoing cost to the treatment plan. Integrating these recurring expenses into a dedicated health budget ensures that the therapy remains effective and that the equipment is well-maintained throughout its operational life.
When considering where to source equipment and services, comparing local providers is a practical step to find the right balance of support and price.
| Product/Service | Provider | Cost Estimation |
|---|---|---|
| Home Sleep Test | EdenSleep | $199 - $350 |
| Auto CPAP Machine | ResMed NZ | $1,600 - $2,400 |
| CPAP Mask | Fisher & Paykel | $220 - $480 |
| Clinical Consultation | Local Clinics | $150 - $300 |
| Annual Consumables Kit | Various Providers | $100 - $250 |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Effective management of sleep-related breathing disorders is a long-term commitment that requires both clinical and financial planning. By understanding the diagnostic costs, equipment price ranges, and the availability of government support in New Zealand, patients can make informed decisions that support their health goals. While the initial costs can be substantial, the benefits of improved sleep quality and reduced long-term health risks often outweigh the financial investment. Engaging with local specialists and staying informed about funding changes will help ensure that therapy remains accessible and sustainable for years to come.